Aaah, those leisurely Saturday mornings. More recently, mine began over coffee while perusing through the latest edition of the OSS weekly digest. Being a dentist, I’m always on the lookout for articles featuring dentistry related topics, and my interest was piqued by a recent feature on treating cavities without drilling. This approach comprises a chemomechanical method, whereby cavities are simply dissolved and scooped away.
Imagine that: never having to hear the high-pitched whine of the dentists’ drill ever again. But like flying horses and leprechauns, some things seem too good to be true, and such is the case here as only certain types of cavities would be amenable to this less invasive chemical treatment. Many more can’t escape the drill, as they are situated between the teeth or under old amalgam or white resin restorations. However, dentophobes need not despair, as more Quebec dentists have adopted a recent paradigm set forth by faculty members at the University of Laval whose 2015 articles advocate for a shift away from treating all visible signs of tooth decay towards non-invasive preventive and remineralization measures.
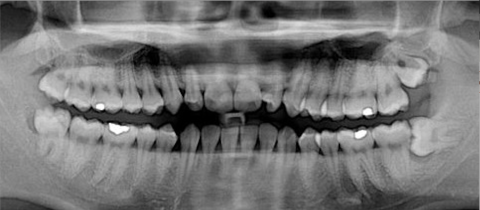
For dentists, seeing that smile of relief on patients’ faces after telling them they have no cavities never gets old. So, it’s never easy to explain how after having had three consecutive perfect check-ups they have some tooth decay. “How could that be?” is the usual response. Typically, most people have routine dental X-rays taken every fourth visit, or roughly every two years. And it is through this means that dentists are able to identify previously undetected cavities between the teeth. These surfaces are harder to clean and despite assurances to the contrary, we know that many of our patients do not floss. Being tightly wedged against one another, and usually located mid tooth, these lesions are only accessible by drilling slot preparations through what is often healthy enamel. And that has long been a challenging paradox facing the dental profession.
Being trained in the principles of tooth conservation, dentists have long struggled with the concept of drilling into healthy tissue in order to access and remove decay. Until recently, with prevention being a fundamental guiding philosophy of the profession, dental students were taught to remove any visible sign of disease surgically, regardless of how far it had progressed into tooth structure. Aiming to prevent decay from spreading through hard enamel to softer, more vulnerable dentin, and heaven forbid, the pulp, dentists routinely drilled into sound enamel in order to reach the infected tissue. While weighing the potential risks/rewards when deciding whether to treat or not treat an affected tooth, clinicians more often than not chose the nip it in the bud restorative approach. But that’s changing.
The 21st century has seen some significant advances in the study of tooth decay, highlighted in a 2002 publication by the California Dental Association. Based largely on these as well as more recent studies, a team from University of Laval's Faculty of dentistry advocate, in general, for the non-surgical treatment of carious lesions that have not extended beyond the dentin-enamel junction. In its place, these smaller cavities should be the object of remineralization treatment. To achieve this, patients can be prescribed a variety of chemotherapeutic agents, most notably a toothpaste with a higher concentration of fluoride, specifically 5000 ppm compared to the usual 1000-1400 ppm found in common brands. Using a pea size amount once/day, combined with an additional brushing using regular toothpaste, not only can existing tooth decay arrested, but remineralization of carious lesions, as evidenced by follow-up radiographs, can be achieved.
Unlike fluoride found in drinking water, which largely gets incorporated into developing teeth, this effect is topical, with the chemical agent penetrating into and strengthening teeth that are fully formed. To prevent inadvertent ingestion, this treatment is not recommended to patients younger than sixteen. Fortunately, there are other non-surgical alternatives in treating decay for pediatric patients.
While other risk factors including oral hygiene habits, diet and past history of dental caries must all be carefully considered when deciding which treatment is best suited to individual patients, dentists now have at their disposal a non-invasive approach to help in our never-ending battle against tooth decay. And that should give patients reason to smile!