A retinal detachment is a medical emergency and if it is not assessed and treated you may lose all the vision in the affected eye.
Retinal detachment occurs when the sensory retina separates from the retinal pigment epithelium rather like wallpaper peeling off a damp wall. The retina needs to be attached to the pigment epithelium to survive and work properly, so if a retinal detachment is not detected and treated quickly it can result in the loss of some or all the vision in your eye.
How your eye works
When you look at something, light passes through the front of your eye, and is focused by the lens onto your retina. The retina is a delicate tissue that coats the inside of your eye. The retina converts the light into electrical signals that travel along the optic nerve to your brain. The brain interprets these signals to "see" the world around you. The retina is made up of different layers. The sensory retina contains the light sensitive cells and its supporting layer is made up of the retinal pigment known as epithelium. The retina is also supplied with blood by a delicate network of blood vessels on its surface.
Light is focused onto a tiny area of the retina called the macula, which is about the size of a pinhead. This highly specialised part of the retina is vital, because it enables you to see fine detail when you are looking directly at something such as words, photos or the television. Your macula also gives you much of your ability to see colours. The rest of the retina, gives you side vision (peripheral vision). The eye is filled with a clear substance called the vitreous gel. Light passes through the gel to focus on the macula.
Causes
Most retinal detachments happen because a tear or hole in the retina allows fluid to leak between the retinal layers and this then causes the retina to detach. Holes in the retina can occur because of changes that happen as we age, whereas tears happen because the retina

Other eye conditions such as diabetic retinopathy can result in fibrous scar tissue forming inside the vitreous and on the surface of the retina. This scar tissue can then pull on the retina (traction) causing a detachment. This type of traction on the retina can also cause tears that allow the fluid to leak in between the layers, again causing a detachment. This type of retinal detachment is called Tractional.
Fluid from the vessels behind the retina can also leak between the retinal layers. This is a less common cause of detachment and happens because of another condition such as an inflammation or tumour. This type of retinal detachment is called Exudative.
Who is at risk?
Rhegmatogenous retinal detachment is the most common form of retinal detachment and is still very rare. It only occurs in about 1 in 10,000 people each year. Retinal detachment can happen to someone of any age but is very rare under the age of sixteen and most commonly happens to people aged between 60 and 70 years.
Most retinal detachments occur because of a tear in the retina. A common cause of tears is a complete or acute posterior vitreous detachment . This happens when the vitreous gel filling the eye liquifies and collapses. Changes to the vitreous gel are very common in older people, occurring in 60 per cent of people over 70 years of age. For the vast majority of people these changes do not result in any serious complications. For more information, go to our pages on Posterior vitreous detachment. In a small number of cases the pulling away of the vitreous causes a retinal tear and in some cases this can lead to a retinal detachment.
The retina changes as we age and at its edges it can develop holes and weakened areas. These holes can, in some cases, lead to detachment. Holes are far less likely to lead to a detachment than a retinal tear. You have an increased risk of retinal detachment if you:
- are very short sighted (more than minus 6.00 D)
- have had a trauma (injury or blow) to the eye
- already have had a detachment in one eye
- have a family history of retinal detachment.
Symptoms that warn of a retinal detachment
Flashing lights
Many people experience flashing lights, most commonly around the edges of their vision. Flashing lights occur when the retina is stimulated by something within the eye rather than by the light entering the eye. They are often caused by the vitreous gel inside the eye moving and pulling on the retina.
In many cases flashing lights are caused by a gradual vitreous detachment and in most cases this doesn't cause any long term problems with your vision. However, flashing lights can indicate that there is a tear in the retina. There is no way you can tell whether your flashing lights are caused by your vitreous or by a retinal tear. If you suddenly experience flashing lights you should have your eye examined by an optometrist (optician) as soon as possible, usually within 24 hours.
Floaters
Floaters are caused by debris in the vitreous casting a shadow on the retina. The brain then sees this as an object floating around in space. Floaters are very common and we can all expect to have a few as we get older. People who are short sighted or have had eye operations in the past often have more floaters. Floaters can take many shapes being described as rings, spiders' legs or cobwebs. They are not in themselves a cause for concern especially if they have been present for months or years.
However, if you experience a recent dramatic increase in the number of floaters or notice showers of dust-like floaters, this could be a sign that changes are happening at the back of your eye.
If you experience a recent onset of floaters or change to the nature or numbers of your floaters, you should have your eyes examined by an optometrist as soon as possible usually within 24 hours.
Dark shadow
If your retina does detach then it can't work properly anymore. You will see this as a dark shadow in the corner of your vision. If more of your retina detaches then the shadow will move towards the centre of your vision.
If you experience a dark shadow moving up, down or across your vision you need to attend your local eye clinic as soon as possible within the same day if possible or within 24 hours.
Blurring of vision
Your vision can gradually become blurred for many reasons and a visit to the optometrist will help you find out why. If your vision suddenly becomes blurred, especially if any of the other symptoms of flashing lights, floaters or a shadow are present, then this is more serious, and you need to consult your optometrist as soon as possible and usually within 24 hours.
Many people have flashes and floaters and this is normal for their eye. Not every person with flashes and floaters will develop a retinal detachment. However, if you do experience flashes or floaters for the first time, or your usual flashes and floaters change, then you should have your eyes examined.
If you experience a dark curtain or a sudden blurring of vision then this should always be checked as soon as possible preferably at an eye hospital.
If you have been checked for retinal detachment in the past you should have been given clear instructions on what to do if you have further symptoms and you should follow these. This usually involves contacting the hospital eye clinic if you have any concerns.
Prevention
If you have a healthy retina then there is no treatment that can reduce the risk of a detachment. Regular eye tests are an important way to make sure your eyes are healthy and you have no signs of any eye conditions. Everyone should have their eyes tested at least every two years.
One of the main causes of retinal detachment is trauma to the eye. Wearing eye protection for DIY, gardening or sport is something you can do to reduce the risk of an eye injury. Retinal detachment does not happen as a result of straining your eyes, bending or heavy lifting.
If you do experience symptoms of flashes and floaters and the eye clinic detects a hole or tear in your retina then this may be treated to reduce the risk of a retinal detachment developing. Not all tears or holes need treating. The treatment for retinal tears and holes is
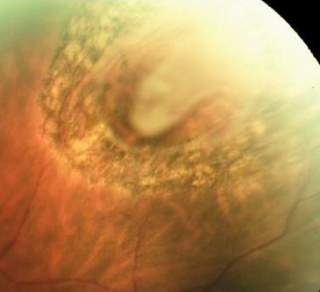
The treatment can be done two different ways, either using a cryoprobe which freezes the tiny area of the retina around your retinal tear or hole from the outside of the eye, or by using a laser which causes very small burns in the area around your retinal hole or tear. The retinal tear or hole is surrounded by the treatments and this prevents it expanding into a detachment.
You can have this type of treatment as an outpatient using a local anaesthetic. Your vision is not usually affected by this type of treatment because only a very small localised area of the retina is treated.
Treatment
Retinal detachment can be treated. The treatment involves an operation to reattach the sensory retina to the underlying retinal pigment epithelium. The sooner treatment is carried out, the better the likely results. If retinal detachment is not treated then you will lose all the vision in the affected eye.
Surgery for retinal detachment is complicated and very individual to each case. The type of treatment needed depends on the type of detachment and any complicating factors, such as any other eye conditions you may have.
After an initial assessment, the specialist eye surgeon (ophthalmologist) will decide how quickly surgery needs to be carried out - this maybe within 24 hours or within a few days. Usually, only one operation is needed and the types of surgery described below may be combined. You will have a local anaesthetic, meaning that you will be awake but feel nothing in your eye. Most people go home the same day as the operation but some people may need to stay in hospital for a day or two.
Pneumatic retinopexy, simple gas bubble surgery
If the retinal detachment is small and uncomplicated, a gas bubble can be injected into the vitreous of the eye. This bubble then presses the retina back in place. The gas is reabsorbed over a period of weeks and the retina remains in place. Depending on the size and position of the bubble, your vision may be very blurred in the first few weeks.
Scleral buckle
If the retinal detachment is more extensive, then a sclera buckle may be used. This involves attaching a tiny piece of silicon, sponge or harder plastic to the outside of the eye. This presses on the outside of the eye, causing the inside of the eye to slightly move (buckle) inwards pressing the retinal pigment epithelium against the detached sensory retina which helps the sensory retina to reattach. Cryotherapy or laser treatment may be used to seal the area around the detachment. The buckle is usually not removed and is not visible once surgery is finished.
Vitrectomy
If the retinal detachment is extensive or has complicating factors such as scarring or bleeding inside the vitreous, then you may have to have a vitrectomy. This procedure involves removing the vitreous gel and replacing it with either a clear solution or a gas bubble. The liquid or gas bubble then holds the detached sensory retina against the retinal pigment epithelium from the inside.
After your operation
After the operation your eye will feel uncomfortable. There may be some bruising and your eyelids maybe sticky. You will be given eye drops to help prevent infection and to control any swelling. Your eye may be uncomfortable for a few weeks after the operation.
First few weeks after the operation
If you have had a gas bubble put into your eye, your vision will be very blurry for a while. This is only temporary. As the gas is absorbed you may see a wavy line across your vision which is the divide between the gas and liquid content of the eye. This will slowly move and then disappear over a period of weeks.
Even without a gas bubble your vision may be blurry for a number of days possibly weeks following the surgery. During this time although your sight will be blurry you don't have to limit how much you use your eyes, so watching TV or reading will not cause any problems.
Your ophthalmologist will tell you which activities you should avoid directly after your operation and the advice may be different depending on the type of surgery you have had. Most people will have some restriction for the first six weeks after the operation.
Once your eye has healed from the operation you can continue the sports or activities you enjoy, but your ophthalmologist is the best person to let you know if any of your regular activities should be avoided in the long term. Usually full contact sports which may involve a blow to the head such as boxing, kick-boxing and martial arts aren't recommended for someone who has had a retinal reattachment surgery
Your ophthalmologist is the best person to give you advice about any activity you need to avoid either just after your surgery or in the long term.
Posturing
Posturing is lying or sitting with your head in a certain position. You may be asked to do this before surgery to stop a retinal break spreading, or after your operation to help keep a gas bubble or the clear solution in place, so that it continues to put pressure on the part of the retina being reattached. You may need to do this for up to ten days after the operation. If you need to do this the medical team will explain how to lie or sit and for how long.
If possible, you may find it useful to have someone to help you at home while you are posturing, but if that is not possible and you are worried about coping, you might want to let your ophthalmologists or GP know about your circumstances as they may be able to arrange for some help.
You need to tell your clinic if you need to fly after having surgery, especially if a gas bubble has been used, as it is not safe to fly until the gas bubble has been completely reabsorbed. If you are having any other operations, the anaesthetist needs to know that you have a gas bubble. Once any period of posturing is finished you can resume normal activities, including sex, as soon as possible.
How successful is treatment?
Surgery is usually very successful at reattaching the retina. The degree to which your detailed and peripheral vision will be affected is likely to depend on how much of the retina detached, if the maculae was detached, if you have another eye condition such as diabetic retinopathy and how quickly the surgery was carried out.
If the macula, which allows us to see fine detail, remained attached then results are often very good and your central vision may not be affected at all. If the macular had detached but treatment was carried out quickly then central vision can return but it may be distorted and wavy. Many people find they adapt to this distortion with time.
If you had a shadow in your peripheral vision, this will disappear after surgery but you may have some restriction to your peripheral vision. The longer the detachment was left untreated and the more extensive it is, the worse the vision is likely to be after the operation.
Unfortunately for some people, their operation may be successful at reattaching the retina but it may not bring back detailed central vision or areas of peripheral vision. This can happen in any circumstance but the risk is higher the longer the retina has been detached without any treatment.
What happens if the detached retina is not put back in place?
Most people will lose all useful vision if no operation is carried out, or if the treatment is unsuccessful. However, if the first operation does not succeed, it is usually possible to have one or more operations to re-attach the retina. At each stage, your surgeon will discuss with you the likelihood of success and the need to have more treatments.
What if my sight is not as good as before?
If you have lost vision in one eye due to a detachment you may still have useful vision in your remaining eye. It can sometimes take a few months to get used to seeing with only the one good eye as the other eye interferes. With time the brain learns to ignore the poorer vision in most situations.
If the affected eye was your good eye then you may be left with a sight impairment. You can receive help to see many of the things you used to see by making use of your remaining sight. Low vision services can help find the best magnifiers for you, and give advice and training about the many, often simple, ways that you can make the most of your sight.